Eczema Treatment in Tampa & Dade City, FL
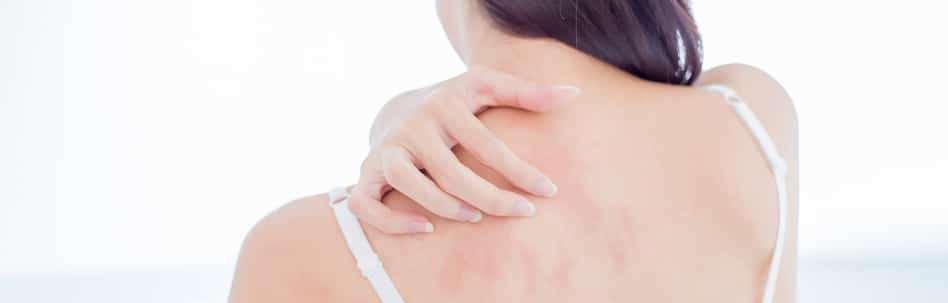
Eczema is a common skin disorder that manifests itself as itchy skin and a red rash; it is particularly common in infants and young children. Eczema most often develops as a result of an allergic reaction, or an immune-system malfunction. It can cause irritation and inflammation anywhere on the body, but is especially prevalent on the face, the insides of the arms, and behind the knees. In infants with eczema, the scalp is frequently affected.
Atopic dermatitis is the most common, chronic, and severe form of eczema. It occurs most often in those with other allergic conditions, such as asthma or hay fever, and who have family members with the same issues. Eczema is not contagious even with direct skin-to-skin contact.
Give us a call at 813-877-4811 today if you wish to speak with our doctors and learn whether you are a candidate for eczema treatment!
Causes of Eczema
While the precise cause of eczema is unknown, certain substances or circumstances can trigger symptoms in susceptible individuals. Patients with eczema may have adverse skin reactions to many common household products, such as soaps, perfumes, lotions or detergents, as well as to animal dander. They may also develop eczema outbreaks as a result of upper respiratory infections. In some cases, eczema may occur from a food allergy.
Although eczema is quite common in infants, most outgrow it by the age of 2. For infants prone to outbreaks, it is best to avoid using products or fabrics that may irritate their skin, and to avoid feeding them foods that seem to precipitate reactions. For adults, too, the best treatment for eczema may be prevention. By avoiding triggers such as coarse fabrics, extreme hot or cold, animal dander and certain soaps or detergents, patients may be able to keep outbreaks at bay. Although stress is often a factor that worsens the condition, eczema itself, with its discomfort and displeasing appearance, can also be a cause of stress.
Symptoms of Eczema
Eczema usually appears as a red rash on the skin, and can include the following symptoms:
- Raised crusty patches
- Blisters that ooze
- Dry or scaly skin
- Itching
Skin discoloration can also be a symptom of eczema.
Diagnosis of Eczema
Eczema is diagnosed by physical examination and patient consultation. It is important that, in addition to a full patient history, the attending doctor take a full family history. Because many people with eczema often have other allergies, allergy tests may be prescribed or performed so that possible triggers can be targeted.
Treatment of Eczema
There are several treatments available to ease the discomforts of eczema. Cold compresses and over-the-counter preparations to address itching may be recommended. If symptoms persist or become more severe, stronger medications may be prescribed. It is important to treat eczema symptoms because the condition breaches the integrity of the skin, allowing bacteria to invade and cause infection. Itching has to be addressed because scratching can lead to crusting and scabbing of the skin, further breaking down tissues, and increasing the risk of infection. Treatment of eczema may include the following:
- Antihistamines
- Topical corticosteroids
- Changes in bathing and laundering habits
- Antibiotics (if infection is present)
- Phototherapy
- Immunomodulators (such as cyclosporine)
Because both phototherapy and immunomodulators have been linked to an elevated risk of cancer, they are usually prescribed only during severe flareups, and for children older than 2 years of age.
Schedule your Eczema Consultation In Dade City & Tampa!
Be sure to fill out our contact form if you wish to book a one-on-one Eczema appointment with Dr. Michael A. Scannon and Dr. Stefanie Altmann. You can also dial 813-877-4811 for our Tampa, FL office, or 352-567-3563 for our Dade City office.
