Psoriasis is an autoimmune disorder that is resistant to treatment and often shows frequent relapse. Prompt and proper treatment from an experienced dermatology provider can mean the difference between relief and prolonged suffering.
The experts at Florida Westcoast Skin and Cancer Center are highly trained in various treatments for this condition and look forward to helping you manage your symptoms and return to a better quality of life.
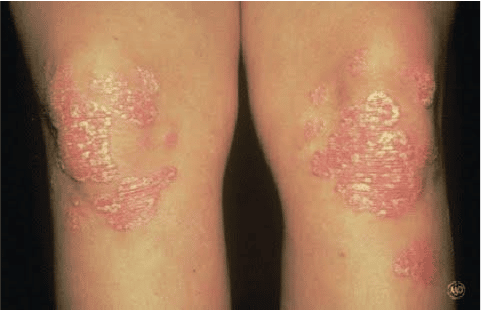
Plaque Psoriasis
About 80% to 90% of people who have psoriasis develop this type. When plaque psoriasis appears, you may see:
- Patches of thick, raised skin called plaques
- Scales (a dry, thin, and silvery-white coating) covers some plaques
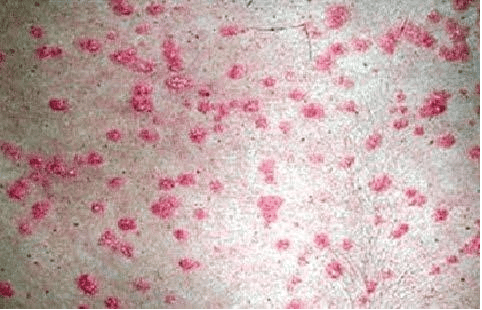
Guttate Psoriasis
This type of psoriasis comes on suddenly and often results in tiny bumps on the skin-often located on the torso, legs and arms but can even be found on the face, scalp, and ears. When these bumps appear, they tend to be:
- Smallandscaly
- Salmon-colored to pink
- Temporary, clearing in a few weeks or months without treatment
Guttate psoriasis tends to develop in children and young adults who have had an infection, such as strep throat. It is possible that when the infection clears so does guttate psoriasis and it may never return. However, in other instances, it is possible for it to last for the remainder of a patient’s life and could potentially later lead to plaque psoriasis.
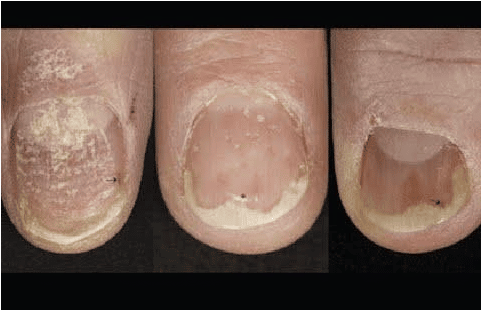
Nail Psoriasis
While many people think of psoriasis as a skin disease, you can see signs of it elsewhere on the body. Many people who have psoriasis see signs of the disease on their nails. About half of the people who have plaque psoriasis see signs of psoriasis on their fingernails at some point.
When psoriasis affects the nails, you may notice:
- Tiny dents in your nails (called “nail pits”)
- White, yellow, or brown discoloration under one or more nails
- Crumbling, rough nails
- A nail lifting up so that it’s no longer attached
- Buildup of skin cells beneath one or more nails, which lifts up the nail
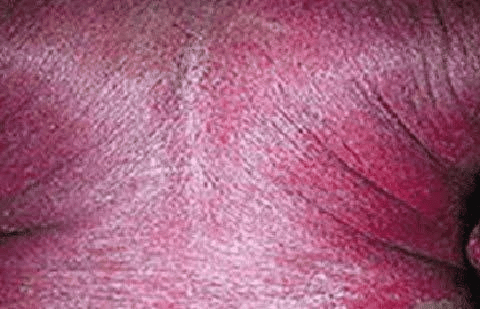
Erythrodermic Psoriasis
Serious and life-threatening, this type of psoriasis requires immediate medical care. When someone develops erythrodermic psoriasis, you may notice:
- The skin on most of the body looks burnt
- Chills, fever, and the person looks extremely ill
- Muscle weakness, a rapid pulse, and severe itch
Most people who develop erythrodermic psoriasis already have another type of psoriasis. Before developing erythrodermic psoriasis, they often notice that their psoriasis is worsening or not improving with treatment. People who develop erythrodermic psoriasis should seek immediate medical attention.
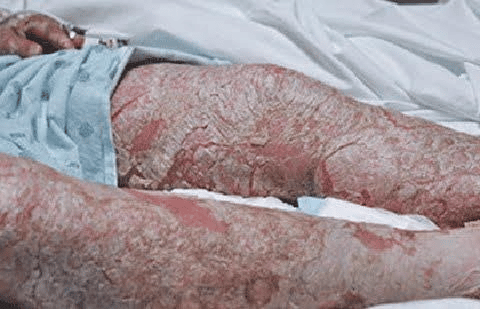
Generalized Pustular Psoriasis
Serious and life-threatening, this rare type of psoriasis causes pus-filled bumps to develop on much of the skin. Also called von Zumbusch psoriasis, a flare-up causes this sequence of events:
- Skin on most of the body suddenly turns dry, red, and tender
- Within hours, pus-filled bumps cover most of the skin
- Often within a day, the pus-filled bumps break open and pools of pus leak onto the skin 4. As the pus dries (usually within 24 to 48 hours), the skin dries out and peels
- When the dried skin peels off, you see a smooth, glazed surface
- In a few days or weeks, you may see a new crop of pus-filled bumps covering most of the skin, as the cycle repeats itself
Anyone with pustular psoriasis will also feel very sick, and may develop a fever, headache, muscle weakness, and other symptoms. Medical care is often necessary to save the person’s life.
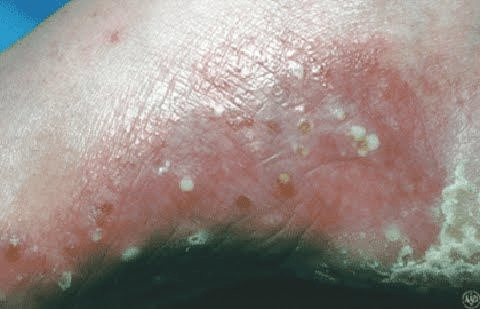
Pustular Psoriasis
This type of psoriasis causes pus-filled bumps that usually appear only on the feet and hands. While the pus-filled bumps may look like an infection, the skin is not infected. The bumps don’t contain bacteria or anything else that could cause an infection. Where pustular psoriasis appears, you tend to notice:
- Red, swollen skin that is dotted with pus-filled bumps
- Extremely sore or painful skin
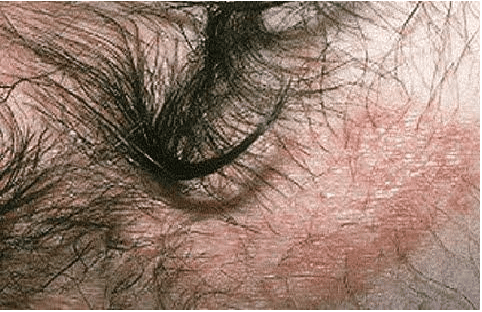
Inverse (Flexural) Psoriasis
This type of psoriasis develops in areas where skin touches skin, such as the armpits, genitals and crease of the buttocks. Where inverse psoriasis appears, you’re likely to notice:
- Smooth, red patches of skin that look raw
- Little, if any, silvery-white coating
- Sore or painful skin
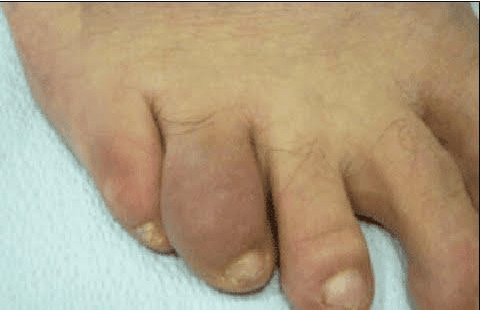
Psoriatic Arthritis
When psoriasis affects the joints, it causes a disease known as psoriatic arthritis. This is more likely to occur if you have severe psoriasis. Most people notice psoriasis on their skin years before they develop psoriatic arthritis. When psoriatic arthritis develops, the signs can be subtle. At first, you may notice:
- A swollen and tender joint, especially in a finger or toe
- Heel pain
- Swelling on the back of your leg, just above your heel
- Stiffness in the morning that fades during the day
Like psoriasis, psoriatic arthritis cannot be cured. Treatment can prevent psoriatic arthritis from worsening, which is important. Allowed to progress, psoriatic arthritis can become disabling.
Information and images sourced from the American Academy of Dermatology (aad.org).

